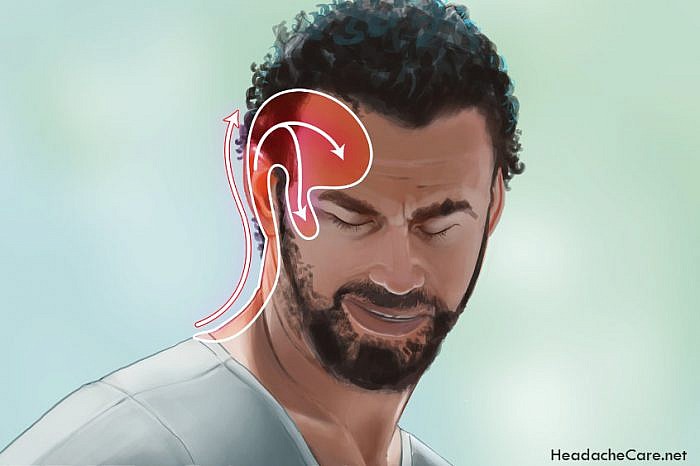
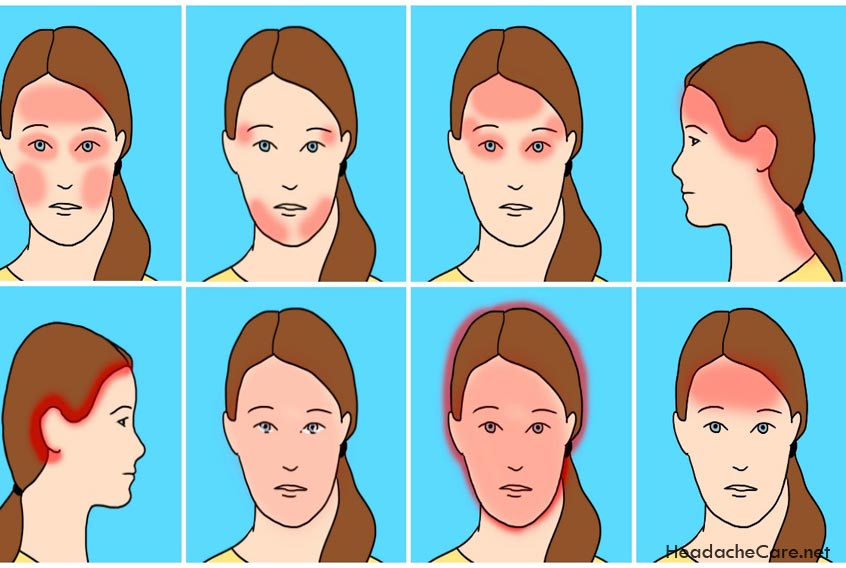
Women are more susceptible to migraines
When women say they endure more pain than men, some people think it’s mostly in their heads.
They might be right.
Almost 30 million Americans suffer from the disabling headaches called migraines. Three out of every four are women.
You can blame hormonal fluctuations for some of that, says Maria Carmen-Wilson, a University of South Florida neurology professor and medical director of the Headache and Pain Center at Tampa General Hospital. Menstrual cycles and other biological changes can trigger the throbbing pain, as can stress, noise or even the weather, she says.
Migraines, which have no discernable medical cause, are not as common as other less-serious headaches, but they get more attention for their ability to knock people out of commission. Symptoms include throbbing pain on one or both sides of the head, nausea, vomiting and sensitivity to light and sound, says the Office on Women’s Health in the Department of Health and Human Services.
Wilson, a speaker at the free Focus on Females health symposium March 27 at the Tampa Convention Center, says she can always spot an invincible superwoman with a migraine.
“It’s the one time when they don’t care about their BlackBerry or Palm Pilot,” she says. “The world can come to an end, and they don’t care.”
[email protected] Some women suffer migraines only once in a while. For others, it’s a chronic problem; they deal with a nearly constant background headache. Anyone who has two or more distinct headaches a week or takes daily over-the-counter pain relief should seek preventive treatment, Wilson says.
Some women suffer migraines only once in a while. For others, it’s a chronic problem; they deal with a nearly constant background headache. Anyone who has two or more distinct headaches a week or takes daily over-the-counter pain relief should seek preventive treatment, Wilson says.
Wilson suggests that people worried about migraines ask themselves some critical questions about their symptoms, such as: Are you missing work or unable to concentrate? Do you need to keep your eyes closed? Do you try not to talk or recoil if someone tries to touch your head?
If so, start a journal tracking your headaches and hormonal cycles. Include eating and sleeping patterns as well as the weather, which also can be a migraine trigger.
“You really can tell a lot from a diary,” says Wilson, who requires all of her Headache Clinic patients to keep one.
Treatments can include more than a prescription. They can range from learned breathing and relaxation techniques to knowing to cut back on headache-inducing red wine when you’re at higher risk for migraines. Lifestyle changes can go a long way toward preventing the disabling pain, she says.
“When people have the attitude of ‘fix me,’ that’s not very good because people have to do their part,” Wilson says. “They have to be engaged. They have to make necessary lifestyle changes.”
WHEN MIGRAINES STRIKE
The likelihood of suffering from migraines fluctuates as estrogen levels fall and rise in the brain, says Maria Carmen-Wilson of Tampa General Hospital. Vulnerable times for female migraine sufferers include:
•Young girls rarely suffer migraines, and when they do, it is at about the same rate as boys.
•First-time diagnosis usually happens around the time of a girl’s first menstrual cycle.
•About 60 percent of women with migraines experience heightened symptoms during their period, but less than 10 percent of women with migraines have them exclusively during menses.
•Pregnancy can significantly reduce the risk of migraines, particularly after the first trimester.
•Birth control pills, which create a steady hormonal release in a woman’s body, can reduce migraine risk for some but not all women.
•Peak migraine risk is between the ages of 35 to 45, the highest time of productivity.
•Migraine sufferers experiencing menopause have it worst, thanks to erratic surges of hormones.
•After menopause, migraines tend to burn out, but hormone replacement therapy may create problems.
For information about the Focus on Females symposium, go to http://www.focusonfemales.com or call (813) 514-4515.
By MARY SHEDDEN